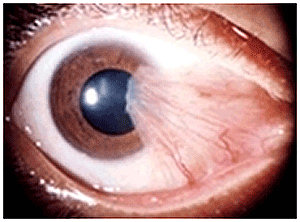
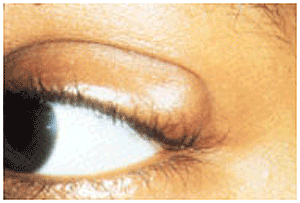
Cataract surgery is the removal of the natural lens of the eye (also called "crystalline lens") that has developed an opacification, which is referred to as a cataract. Metabolic changes of the crystalline lens fibers due to age or trauma lead to the development of the cataract and loss of transparency, causing impairment or loss of vision. Symptoms include: difficulty seeing afar, difficulty reading print, glare, frequent changes to the spectacle prescription, diminishment of colour and brightness. During cataract surgery, a patient's cloudy natural lens is removed and replaced with a synthetic lens to restore clear vision.
If a cataract is suspected or diagnosed, a complete medical eye exam will determine if the cataract needs to be removed. Specifically the clinician will perform Ultrasound size measurements of the eye to determine the most appropriate power for the replacement lens. This intraocular lens (IOL) will reduce the need for glasses and if glasses are required, they will be much thinner and lighter than if an IOL was not implanted.
The primary choices of IOLs are monofocal, multifocal, toric and accommodating. Each has its own advantages and disadvantages. Only after careful discussion with the doctor can the appropriate type of IOL can be selected.
Following surgical removal of the natural lens, an artificial intraocular lens implant is inserted. Cataract surgery is performed by an ophthalmologist in a day surgery or hospital, using local anaesthesia (either topical, peribulbar, or retrobulbar), usually causing little or no discomfort to the patient.
Phacoemusification(Phaco) is the preferred method of removal in almost all cataract operations performed today. It involves a very small incision made in eye and the use of a machine with an ultrasonic handpiece equipped with a titanium or steel tip. The tip vibrates at ultrasonic frequency (40,000 Hz) and the lens material is emulsified.
A second fine instrument (sometimes called a cracker or chopper) may be used from a side port to facilitate cracking or chopping of the nucleus into smaller pieces. Fragmentation into smaller pieces makes emulsification easier, as well as the aspiration of cortical material (soft part of the lens around the nucleus). After phacoemulsification of the lens nucleus and cortical material is completed, a dual irrigation-aspiration (I-A) probe or a bimanual I-A system is used to aspirate out the remaining peripheral cortical material.
The surgery site is then cleaned and prepared for the insertion of the artificial lens. The lens is folded and inserted using a injector and positioned into place.The small incisions do not need stitching and the wound will self seal within minutes of the operation.
The absence of stitches means the visual recovery is fast and there is little discomfort after the surgery. A protective sheild will be positioned over the patient's eye. The complete surgery process will take between 20-40 minutes.
The patient can go home on the same day as the surgery. Transportation home from the surgery needs to be arranged. The patient will be required to use both an antibiotic and steroid drop for approximately 4 weeks following surgery. Recovery is often short within 2 to 6 weeks and complete healing at three months. Some people have noticeable improvement in their vision from the day after surgery onward, while others need more time for their vision to clear.
There is no major restrictions following surgery, however it is advisable not to go swimming for 2 weeks.
Laser cataract surgery is the latest advance.
Here, a femtosecond laser prepares the eye for phacoemusification by making all the wounds, the opening into the front part of the cataract and starts to break up the cataract into pieces. The rest of the operation is then completed as above. Its advocacy is couched in terms of greater accuracy and safety.
YAG laser capsulotomy
A small number of patients may experience capsule thickening months after cataract surgery but more commonly it occurs two or three years after. When the capsule thickens it becomes opaque. This stops the light reaching the back of the eye, as a result vision can be affected and sight becomes cloudy or misty, this will be most obvious at night, or in sunlight.
Laser treatment makes a small hole in the centre of the capsule, and can restore vision to how it was after the cataract operation. This procedure is painless.
The procedure usually only takes a few minutes. Following a YAG laser capsulotomy, normal activities can be continued. The experience of some floaters afterward is normal and these will likely resolve within a few weeks. Most people can expect their vision to improve within a day.
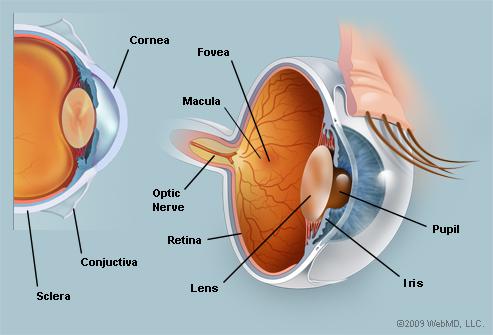 The eye is a slightly asymmetrical globe, about an inch in diameter. The front part of the eye (the part you see in the mirror) includes:
The eye is a slightly asymmetrical globe, about an inch in diameter. The front part of the eye (the part you see in the mirror) includes: